Sleeve Gastrectomy
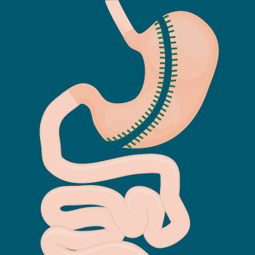 This minimally invasive, though nonreversible, surgery is rapidly gaining popularity among doctors. This procedure generates weight loss by removing a portion of the stomach, decreasing its size by 75 to 80 percent. The remaining stomach takes on a tube or sleeve- like shape, limiting the amount of food that can be eaten at one time.
This minimally invasive, though nonreversible, surgery is rapidly gaining popularity among doctors. This procedure generates weight loss by removing a portion of the stomach, decreasing its size by 75 to 80 percent. The remaining stomach takes on a tube or sleeve- like shape, limiting the amount of food that can be eaten at one time.
Even though the procedure significantly reduces the size of the stomach, it still allows the stomach to function normally. Most food items can be consumed, but in smaller amounts. Research has even shown that a hormone which induces hunger, and is secreted by the part of the stomach which is cut away, will be produced less and appetite will be decreased. For these reasons, many surgeons and patients feel this surgery is superior. The weight loss from this procedure is similar to gastric bypass (and much greater than gastric banding).
Who are candidates for sleeve gastrectomy?
- Body Mass Index (BMI) of 40 or higher, or;
- BMI between 35 and 39.9, with significant obesity-related medical problems
- A long-standing history of obesity with multiple failed attempts at weight loss in the past, preferably with organized, medically supervised programs
- Between 18 and 60 years of age (patients outside this age range may be considered on a case-by-case basis)
- Not be actively smoking or abusing drugs or alcohol
- Commit to long-term follow up and lifestyle modifications
- Laparoscopic sleeve gastrectomy has rapidly gain popularity among surgeons and patients due to very favorable weight loss, low complication rate and less complexity compared to gastric bypass. Nutritional supplements are not needed to the extent typical for gastric bypass. Most patients report significant decrease in hunger despite only eating a small amount of food.
The Surgery
This surgery is performed under general anesthesia and takes about 1 to 2 hours. Since this surgery is laparoscopic, the surgeon will make small incisions in your abdomen instead of one big incision, and insert a special camera and the surgical instruments that will remove part of your stomach. This leaves behind a small, tube-shaped pouch that only holds three to four ounces.
Advantages of Sleeve Gastrectomy:
- Less invasive than gastric bypass
- No rerouting of the intestines
- Stomach empties normally into the small intestine
- Does not require an implanted device that is utilized with gastric banding surgery
- May be better for patients with prior surgery or certain medical conditions
- Fewer complications and malabsorption issues
- Little risk of “dumping syndrome”
- Nutritional supplementation not as great as with gastric bypass
- Rapid weight loss within a year. Weight loss greater than gastric banding surgery
- Weight loss similar to gastric bypass
Risks associated with Sleeve Gastrectomy:
- Leakage of the sleeve (stomach) leading to infection
- The stomach can stretch and weight may be regained over time
- Need for additional weight loss surgery
- Bleeding
- Blood clots (in legs or clots going to lung)
- Anesthesia complications
- Death
Pre-surgery
Stopping smoking has shown to significantly decrease complications and reduce chances of leaks. You are encouraged to begin a healthy diet consisting of smaller, more frequent meals in the weeks leading up to your operation. You should incorporate healthier foods into your diet and exercise more. Doing so will help you launch your healthier lifestyle and possibly lose weight prior to surgery, as well as reduce risks and enhance surgical outcomes.
Post-surgery
Most patients will be hospitalized for only one to two days following surgery. You will be prescribed pain medication to make you more comfortable. While exercise and heavy lifting are not permitted right after surgery, walking is encouraged to prevent blood clots. Many patients can go back to work after only one week. A full recovery can take up to three weeks.
In the first 24 hours you can only drink clear liquids to make certain you have no problem consuming or retaining fluids. You will adhere to a liquid diet including special protein shakes in the two weeks after surgery, followed by two weeks of pureed food before being reintroduced to solid foods. You will be provided with a post-surgery nutrition plan, complete with a vitamin and mineral regimen that should be followed to prevent malnutrition. Our registered dietitians will explain this in great detail before your surgery and again before your discharge.
We are here to assist you along the way, providing encouragement and answering your questions.
For more information...
Contact Ashley Austin, DNP at 229-931-1152 or e-mail ajaustin@phoebehealth.com.